Content
Published:
This is an archived release.
Stable use of general practitioners and emergency primary health care services
In 2013 the population had 2.6 GP consultations on average and the corresponding figure for the use of emergency primary health care services was 0.26; a slight decrease from 2012. While the middle-aged and elderly use general practitioners (GPs) the most, the most frequent users of emergency primary health care services are young children.
| 2013 | ||||
|---|---|---|---|---|
| General practitioner (GP) | Emergency primary health care | |||
| Share of persons | Consultations per person | Share of persons | Consultations per person | |
| All ages | 68 | 2.6 | 17 | 0.26 |
| 0-5 years | 65 | 1.7 | 32 | 0.55 |
| 6-15 years | 53 | 1.1 | 16 | 0.21 |
| 16-19 years | 62 | 1.6 | 20 | 0.29 |
| 20-29 years | 63 | 2.1 | 20 | 0.30 |
| 30-49 years | 67 | 2.6 | 15 | 0.22 |
| 50-66 years | 75 | 3.2 | 14 | 0.20 |
| 67-79 years | 85 | 4.3 | 16 | 0.24 |
| 80-89 years | 82 | 5.2 | 22 | 0.35 |
| 90 years or older | 60 | 3.2 | 21 | 0.35 |
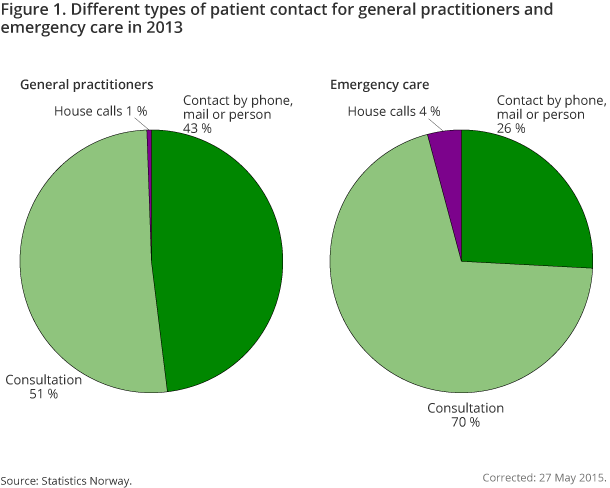
In combination, GP services and the municipal emergency primary health care services make up a significant share of primary health care. However, the GPs’ work with listed patients is far more extensive than for the emergency primary health care services, and the total number of consultations with GPs was 10 times that of the emergency primary health care services in both 2012 and 2013. Consultations with GPs also constituted a somewhat smaller share of the total number of patient contacts that was reported to HELFO (63 per cent) than for emergency primary health care services (70 per cent) as seen in figure 1. The statistics presented here are based on data on consultations, and this is the form of contact referred to throughout the article.
Different age patterns for use of GPs and emergency primary health care services
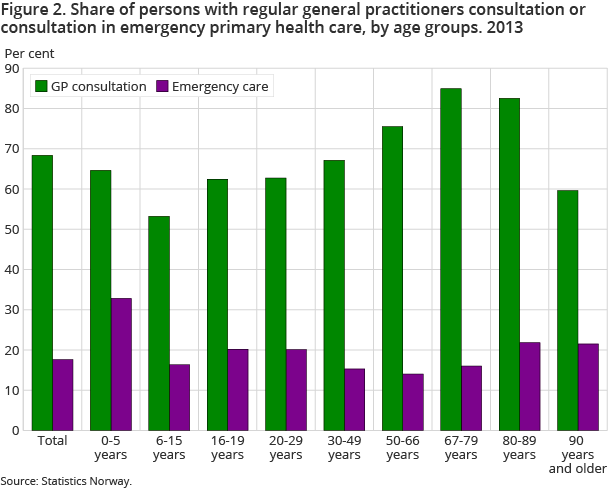
An average of 0.26 consultations per person means that a minority of the population sought municipal emergency primary health care services during the year, i.e. 17 per cent. In comparison, at least one GP consultation was registered for 68 per cent of the population (figure 2). School-age children (53 per cent) had the smallest share of use of GP services and the highest was among patients aged between 67 and 79 years old (85 per cent). The fact that chronic health problems increase with age means that the GPs’ work is largely aimed at the middle-aged and elderly. The fall in the share who visited a GP after the age of 80 is probably not due to better health, but rather that the need for medical care is covered by other means (e.g. doctors at nursing homes).
Infants often suffer from an acute illness, e.g. respiratory infections that develop quickly, and families with children under 6 were most likely to visit the emergency primary health care services in 2013. In this age group, one in three were registered with at least one consultation during the year, while the corresponding figure for young adults under 30 was one in five. The middle-aged and elderly aged under 80 years used emergency primary health care services less than young adults. The share of users of emergency primary health care services among the elderly aged 80 and over, however, was higher than for most other age groups. Thus, this is the opposite of what we see for the use of GPs, where the share falls slightly, especially after the age of 90. It would appear that the oldest and weakest need emergency medical care from the emergency primary health care services as a supplement to the regular medical supervision many of them receive within an institution.
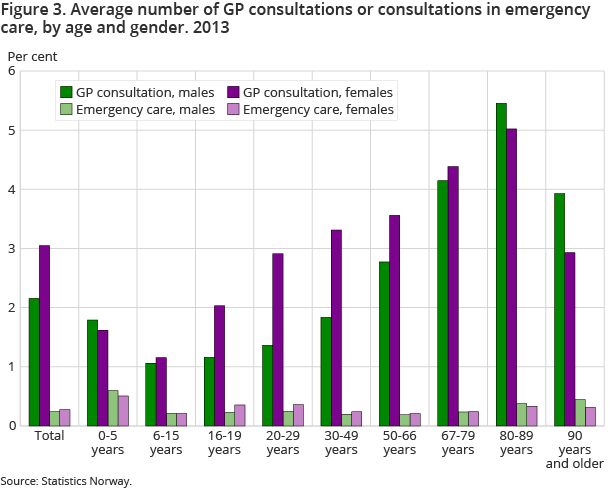
Many GP consultations among men and women in their 80s
Among those who visited the municipal emergency primary health care services in 2013, most had one or two consultations, including the elderly. Among all 80-89-year-old men, the average number of consultations at emergency primary health care services was 0.37. The corresponding average figure for the use of GPs was 5.5, with more than 80 per cent of them visiting a GP more than six times on average. Compared with school-age children with an average of one consultation per year, there were more than five times as many consultations with GPs per person aged between 80 and 89 years. About a quarter of the GP consultations were with the under 30s, while half of the consultations with emergency primary health care services related to this section of the population.
Less use of GPs and emergency primary health care services with higher education
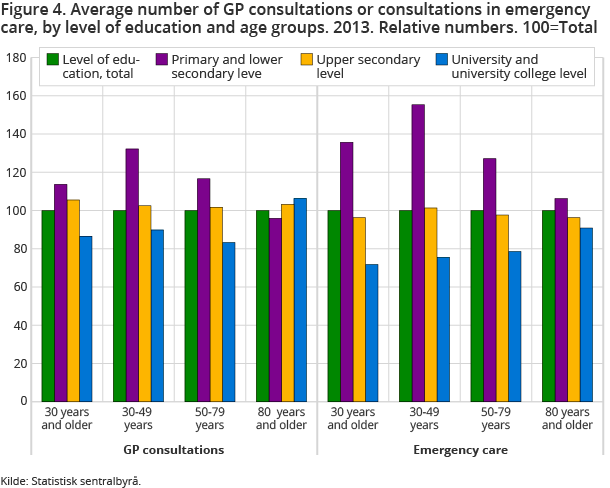
The patterns for use of GP and emergency primary health care services change slightly from year to year. In 2013, it was largely persons with a lower education that visited GPs the most, but the disparities between the education groups decreased with age. Among persons aged over 80, the education effect is reversed, with more use of GPs among the highly educated than among those with a lower education. Use of emergency primary health care services was, on average, slightly more frequent among the lower educated than those with a higher education, among the elderly, as well, see figure 4. There are many possible explanations of the differences between the two patterns described in the figure. One is that use of emergency care has a closer connection with severe illness, whereas contacts with GP sometimes are taken to prevent severe health problems.
Municipal emergency primary health care servicesOpen and readClose
All municipalities are required to provide emergency primary health care services. This entails, among other things, 24-hour emergency telephone cover and a doctor on duty who will provide urgent assistance to anyone living in or located in the municipality (cf. Act relating to the municipal health services of 1984). Many municipalities have chosen to work together, and almost 80 per cent of municipalities have some form of inter-municipal cooperation on emergency primary health care, especially in the evening and at night. Read more in; About the statistics.
Contact
-
Inger Texmon
E-mail: inger.texmon@ssb.no
tel.: (+47) 95 27 50 06
-
Arne Jensen
E-mail: arne.jensen@ssb.no
tel.: (+47) 99 71 22 45
